Information and treatment options for Achilles Tendinopathy / Achilles Tendon pain.

Below we have put together an Achilles Tendinopathy information guide including the most effective treatment options such as, a progressive training program and Shockwave Therapy.
The Achilles tendon is what connects the calf to the heel. It is the strongest tendon in the body but is also one of the most common to have pain from!
Achilles tendon pain is known as Achilles Tendinopathy and used to be called Achilles Tendonitis. It is no longer referred to as an ‘itis’ because ‘itis’ means inflammation and newer research suggests that it is not necessarily inflammation that causes the pain.
There are more than one type of Achilles Tendinopathy and they require slightly different considerations when it comes to treating and managing them.
Mid Portion tendinopathy
Here the pain is 2-7cm above the heel bone and is often painful when pinching it. It is the most common type of tendinopathy
Insertional tendinopathy
The pain is closer to the heel bone where the tendon attaches to the bone. Compression will aggravate it and so stretching the calf should be avoided. It is also important to get the right diagnosis as there are other potential causes of pain in this area.
3 Phases of tendinopathy
There are three main phases of Achilles tendinopathy and these exist on a continuum. The phases are:
- Reactive
- Disrepair
- Degenerative
From a treatment point of view it is good to look at them in two distinct parts
- Reactive/early disrepair
- Late disrepair/ degenerative
Reactive/ Early disrepair
During this phase the most important thing is to manage your activity level to allow the symptoms to settle. It is important to limit the load. Load can be both compressive and tensile.
Jumping, running (especially sprinting) and even walking induce a tensile load in the Achilles tendon. Don’t avoid these activities altogether but manage how much you do so that it doesn’t overly irritate the tendon.
Compressive loads are anything that can compress the tendon. This can include shoes pressing onto the tendon or having the foot in a position of dorsiflexion (when your foot gets closer to the shin). This position occurs when walking uphill for instance and it also occurs when stretching the calf. In the past it has been recommended to stretch the calf/Achilles but recent research has shown that not only is this unlikely to help but it’s possible to aggravate the tendon further.
“Tendons talk 24 hours after a stimulus” so it is not just important to monitor how it feels during an activity or immediately after but for the next 24 hours after that. It may feel fine at the time but hurt the next day. This is known as a latent response.
A reactive tendinopathy can be highly irritable but pain can settle relatively quickly, after a week or so. However it will still be easily aggravated and sensitive to high loads. Therefore once the pain has settled a graded return to activity is required.
How can you reduce the pain of Achilles Tendinopathy?
A form of exercise that can be effective at settling down the symptoms and providing pain relief, as well as helping to maintain strength, is isometric exercises.
The term isometric means the muscle is working but is not changing in length.
Stand on the floor and push up onto your toes. Not all the way up- about half way. Hold this position for 30-60 seconds. Then repeat for 3-4 sets each side. These can be done 3-4 times per day. Start off on both feet but progress to single leg when you are able.
Non steroidal ant-inflammatory medication such as ibuprofen can be used to help relieve reactive tendinopathy. Although it is not inflammation causing the pain, medication can regulate the activity of cells (tenocytes) within the tendon that produce proteins which promote swelling. It is important to note here that long term use is NOT recommended as it can be detrimental to the tendon. Additionally if you are going to take medication make sure you are able to do so and speak to your GP or a pharmacist if you need to.
Late disrepair/degenerative
This is more common as we get older and the tendon can become thicker with nodules in it. There are structural changes that occur within the tendon during this stage. However through a loading exercise regime we can increase the amount of “good” tendon so it doesn’t matter!!! A disrepair/degenerative tendon tends to be a grumbly tendon that has been around for a longer period of time.
Another point just to confuse matters is that you can get a reactive stage in a degenerative tendon after a sudden increase in load. In this instance apply the principles for reactive tendinopathy for it to settle.
It thought that a reason for the disrepair/degenerative tendon to develop is a lack of a complete healing response. The tendon not be strong enough to cope with the demands placed upon it is thought of as the main reason for a degenerative tendinopathy to develop in the first place. Research shows weakness in the calf musculature (both the gastrocnemius and soleus) to be present in people with Achilles tendinopathy. This is compared to healthy (pain free) controls.
The good news is that humans are adaptable and we can use strengthening exercises to make the muscles and tendon stronger.
Strengthening exercises follow a continuum and need to be progressed to be effective. It is not a short term fix and for a disrepair/degenerative tendon the research suggest a 12 week progressive exercise program is required. It is advisable to maintain strengthening into this area as part of your routine to prevent it coming back. The biggest risk factor for developing Achilles tendinopathy is having previously had it. By maintaining strength you are more able to prevent it from coming back.
The Progressive Training Program
Prime Therapy Clinic follow the principals of progression along a continuum of exercises for Achilles tendinopathy. Where an individual starts, where they finish and how quickly they progress along the continuum will vary considerably from person to person. It will depend on current fitness level, symptoms, goals of what they want to achieve etc…
Strengthening exercises are given for both the gastrocnemius and soleus which are the two muscles that make up the calf musculature. Both attach to the foot via the Achilles tendon. In addition sometimes other exercises for muscles in the foot/around the ankle and further up the leg in the glutes are also prescribed as part of the rehabilitation program.
The continuum is as follows
Isometric -> eccentric -> slow concentric -> faster concentric -> plyometric
The exercises to the left of the continuum are performed more often. Typically a few times per day for isometric or once per day for eccentric. However as we progress we increase the load on the tendon and it needs time to recover and adapt from this stimulus. Here the exercises are typically performed three times a week with at least one rest day between treatments.
A couple of examples of home exercises given at different stages of the continuum that are useful when treating an Achilles tendinopathy are:
Isometric exercises
These are typically given for patients with higher levels of pain/irritability to help it settle.
Try to hold for 30->45 seconds for 3->5 sets and perform them 3 times per day.
Eccentric exercises
Stand up onto your tip toes on both legs and then slowly lower down on one leg. Repeat this 12 times for 3 sets on each leg with the knee straight (targeting the gastrocnemius) and then another 3 sets with knee bent (targeting the soleus) Even if the pain is only in one leg it is recommended to do strengthening on both sides. Perform this once per day.
Concentric exercises
Using a Smith machine at a gym put some weight on the bar and standing on 1 leg go up onto your toes and lower back down. Do this for 3 sets of 12 on each leg with the knee straight and 3 sets of 12 on each leg with the knee bent. Perform this 3 times per week with at least one rest day.
If you do not have access to a gym this can be done at home using a rucksack for added weight.
Plyometric exercises
Examples of plyometric exercises that can be integrated into training programs include hopping and skipping.
Treatment Options
Manual Therapy
Our Chiropractor and Sports Therapist offer treatment for Achilles Tendinopathy. As well as a home exercise program we may also perform manual therapy to the joints in the foot, the ankle, the hip and or spine. If there are any tightness or restrictions in these areas it can lead to overload or compensations in the Achilles which may contribute to Achilles tendinopathy.
Manual therapy in the form of muscle techniques are also performed on appropriate musculature.
Shockwave
The first line of treatment for Achilles tendinopathy is a progressive loading program however tendinopathy is often at times very hard to treat and there are occasions when this is not enough. When this is the case a very effective treatment option is Extracorporeal Shockwave Therapy.
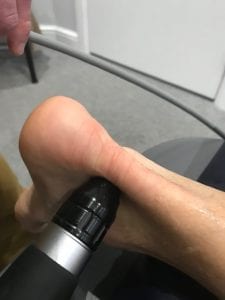
Multiple randomised controlled trials have shown that Shockwave Therapy is an effective treatment for patients with chronic Achilles tendinopathy. It is in the NICE guidelines for when other options have failed to work. For more information on Shockwave Therapy click here
The best treatment for chronic tendinopathy according to research is a combination of loading exercises with Shockwave Therapy. This has been shown via the research to be more effective than either by themselves. It is what we do here at Prime Therapy Clinic!
If you are fed up with the pain of Achilles tendinopathy, then book an appointment with us for the most effective, evidence based treatment available.
